
Scientifica's selection of exciting neuroscience research from May 2020
Included in Scientifica's picks of the best neuroscience research news from May is the development of an artificial intelligence algorithm that can detect different types of brain lesions from CT scans, discovery of a pain-suppression centre in the brain and a new therapy for depression. We hope you find these interesting too!
1. Soft robotic exosuit makes stroke survivors walk faster and further
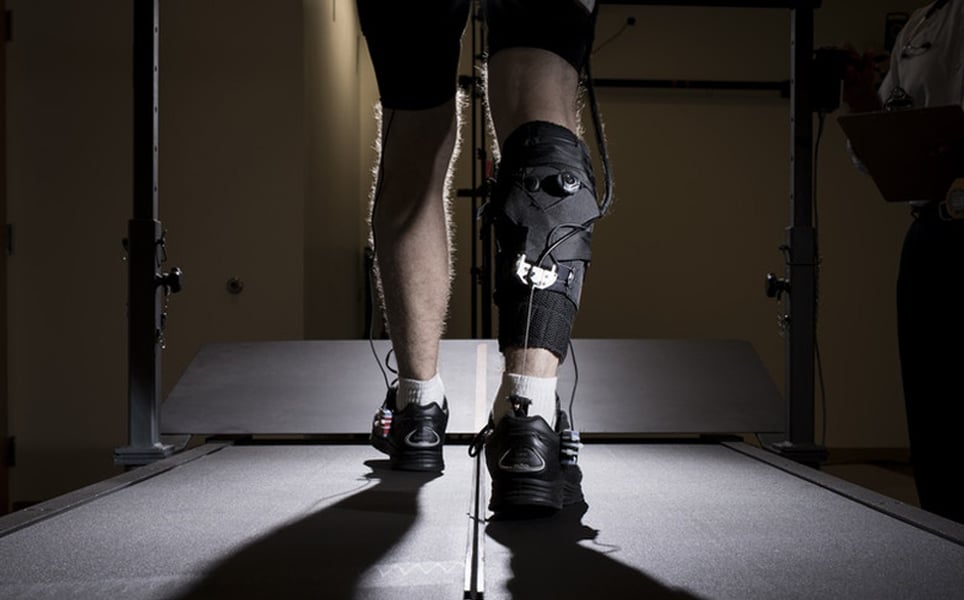
A soft robotic exosuit developed by scientists at Harvard’s Wyss Institute successfully improved the walking speed and endurance of stroke survivors with chronic hemiparesis.
Hemiparesis is a paralysis that affects the limbs and facial muscles on one side of the body, causing severe walking difficulties, loss of balance and muscle fatigue. This exosuit is designed to rehabilitate patients with hemiparesis, with the goal of improving the walking speed and distance that these patients are capable of.
In the study of six post-stroke survivors with hemiparesis, the exosuit increased the walking speed by an average of 0.14 metres per second, with the study participatnts being able to walk an average of 32 metres further in six minutes.
It is hoped that in the future, this exosuit could be used in clinical settings and in the homes of patients to help improve their walking day-to-day.
Learn more
2. The strength of your mental imagery might depend on how 'excitable' your neurons are
Scientists at the University of New South Wales have found that the strength of a person’s mental imagery is linked to the excitability of different regions of the brain.
It was found that highly excitable neurons in the prefrontal cortex made a person more likely to visualise clear images, whereas excitable neurons in the visual cortex reduced a person’s ability to visualise clear mental images. The researchers hypothesise that this is due to more frequent firing of neurons in the visual cortex adding ‘noise’ to the image signal.
Strength of mental imagery
3. AI successfully used to identify different types of brain injuries
An artificial intelligence (AI) algorithm that can detect, differentiate and identify different types of brain lesions from CT scans has been developed by scientists at the University of Cambridge and Imperial College London.
Detailed assessment of a CT scan can take hours. With this tool, different types of brain lesions can be identified and quantified automatically, saving time. It may also be better than a human at detecting changes to injuries over time, enabling the researchers to identify which lesions get larger and progress, as well as gain understanding as to why they progress, leading to the development of more personalised treatment for patients.
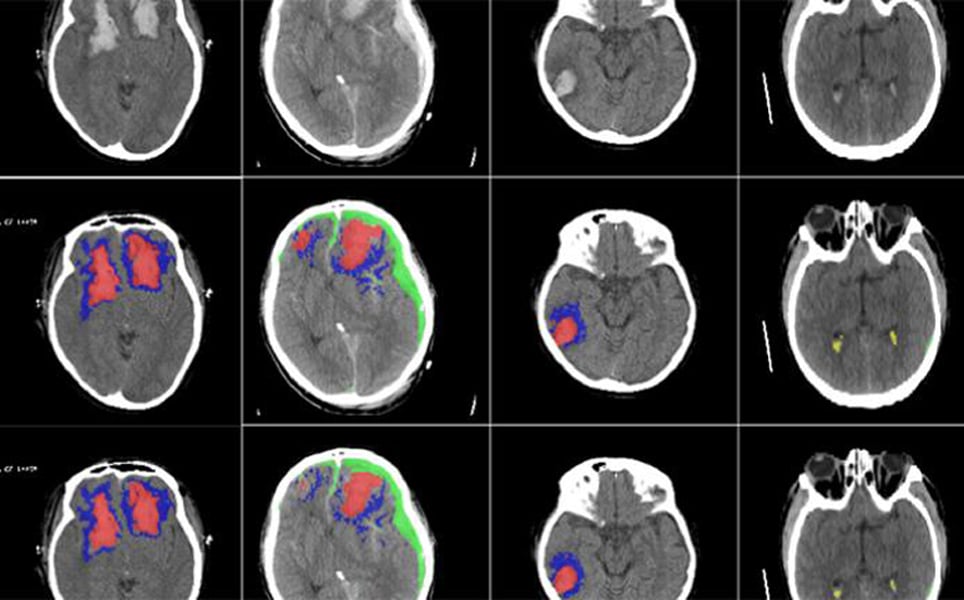
Detection of brAIn lesions
4. Discovery of potent pain-suppression centre in the brain
An area of the brain in mice that is able to switch pain off has been discovered by researchers at Duke University.
This pain-suppression centre is unexpectedly located in the amygdala of the brain, which is known for processing emotions such as fear and the fight or flight response. It was discovered to be involved in switching off pain when the researchers looked at areas of the brain that are switched on by general anaesthetics. They discovered that a subset of inhibitory neurons in the central amygdala, known as CeAga neurons, are activated by general anaesthesia.
The researchers mapped at least 16 brain regions, known to process the sensory or emotional elements of pain, that were receiving inhibitory inputs from CeAga neurons. Optogenetics was then used to activate the CeAga neurons, which led to self-caring behaviours that mice exhibit when uncomfortable being stopped instantly. When the scientists reduced the activity of these neurons, the mice began to act as though they had experienced a painful stimulus again.
Next, the scientists are going to identify any drugs that can activate these CeAga cells in the amygdala only, in order to suppress pain.
Potential new way to suppress pain
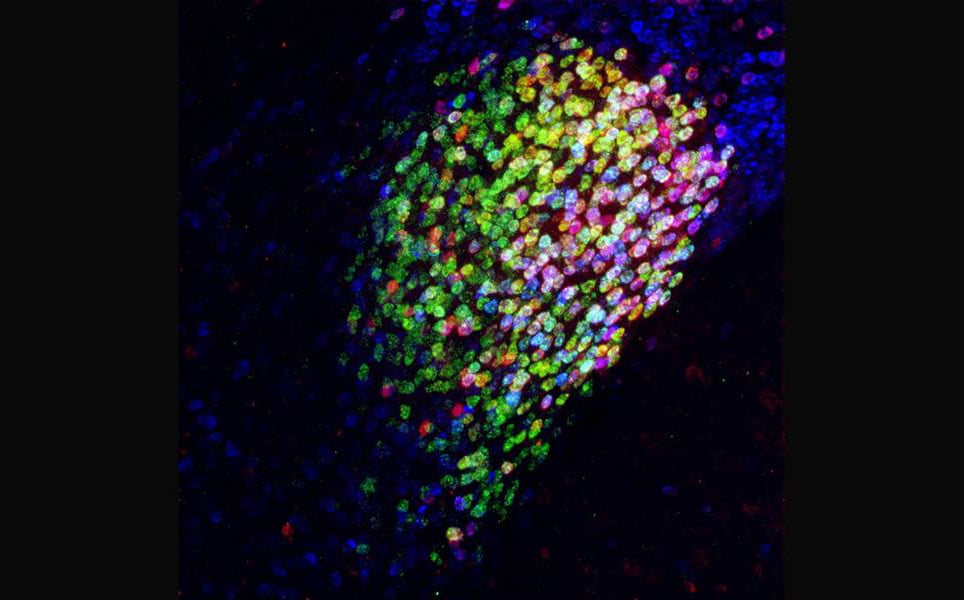
5. Animal study shows human brain cells repair damage in multiple sclerosis
After scientists at the University of Rochester Medical Center transplanted human glial cells into animal models of multiple sclerosis, nerve cell damage was repaired and function restored through remyelination.
The researchers found that when the human glia progenitor cells were transplanted into adult mouse brains, they migrated to where they were needed and created new oligodendrocytes, which are destroyed in multiple sclerosis. The oligodendrocytes then replaced the lost myelin, which led to restoration of motor function in the mice.
This research provides new potential therapeutic options for multiple sclerosis and other neurodegenerative disorders, which can be further explored.
Remyelination in multiple sclerosis mouse model
6. New therapy more effective than CBT for depression
A new therapy developed by scientists at the University of Manchester has been found in a recent study to be better at treating depression that Cognitive Behavioural Therapy (CBT).
The new therapy, Metacognitive Therapy (MCT), aims to change basic mental regulation processes that have become biased, whereas the aim of CBT is to modify thought content.
In the study, which was conducted in Copenhagen, 74% of patients receiving MCT recovered, compared to 52% of patients receiving CBT. This could have a major impact on the treatment of depression, for which CBT is seen as the gold standard.

Could MCT be the new CBT?
7. Scientists find a new way to reverse symptoms of Fragile X
Scientists at MIT have identified a small-molecule compound that may be an effective treatment for Fragile X syndrome.
In a mouse study, using the small-molecule compound to inhibit the GSK3 alpha enzyme reversed many of the behavioural and cellular aspects of Fragile X. The GSK3 enzyme could also be a potential target for Alzheimer’s disease, as it is responsible for phosphorylating tau, which forms tangles in the brains of people with Alzheimer’s.
The compound has now been licensed for further development and potentially human clinical trials. From the mouse studies, it appears that this small-molecule compound doesn’t have the same limitations of other Fragile X drugs that have previously failed human clinical trials.
Small-molecule treatment for Fragile X
8. Yale researchers find where stress lives
Researchers at Yale have discovered that the sensation of stress is generated by neural networks originating in the hippocampus.
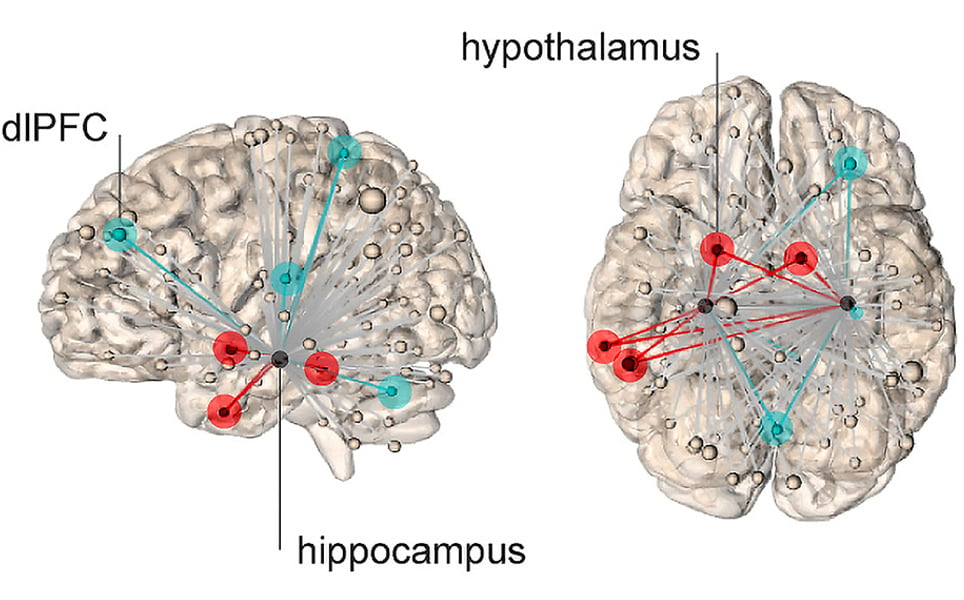
The researchers used fMRI to scan the brains of people exposed to highly stressful and troubling images, and asked subjects to quantify their stress levels when presented with an image. They discovered that the neural networks originating in the hippocampus that are activated when viewing the stressful images reach areas of the brain associated with the physiological stress response, as well as the dorsal lateral frontal cortex, which is an area of the brain involved in higher cognitive functions and regulation of emotions.
When neural connections between the hippocampus and frontal cortex were stronger, the subjects felt less stressed by the images, whereas, when the connections between the hippocampus and hypothalamus were active, they felt more stressed.
These findings may help therapeutics for mental health disorders such as anxiety to be developed. It may allow interventions that increase the strength of connections between the hippocampus and frontal cortex, or decrease the signals between the hippocampus and hypothalamus to be developed.
Find out more
9. New method provides unique insight into the development of the human brain
A new research model of the early embryonic brain has been developed by scientists at Lund University. This model will enable the earliest stages of human brain development to be studied to understand how different regions are formed.
The model, called MiSTR (Microfluidic-controlled Stem cell Regionalisation) was created using stem cells, which are cultivated in a custom-built cell culture chamber that exposes them to an environment resembling the environment in the early embryonic brain. This enables the model to successfully mimic the early developmental stages of the human brain, with tissue of different brain regions next to each other, similar to an embryonic brain.
With new insights into embryonic development, and how neural cells are formed, the researchers are hoping they will be able to more efficiently produce different neural cells for the treatment of neurological diseases. The team are also hoping to be able to create a complete map of human brain development, which will speed up the development of new stem cell treatments.
New insight into human brain development
10. Complement genes add to sex-based vulnerability in lupus and schizophrenia
Variants of a complement gene, part of the immune system, cause men and women to have different vulnerabilities to the autoimmune diseases lupus and Sjögren’s syndrome, according to researchers at the University of Alabama at Birmingham.
These gene variants have also previously been found to potentially increase the risk of schizophrenia. It was already known that all three illnesses were associated with the major histocompatibility complex (MHC), a region on chromosome 6 which encodes many genes that regulate the immune system. However, the researchers have now identified the complement alleles C4A and C4B as those that increase the risk of developing the illnesses.
It was found that different combinations of C4A and C4B copy numbers alter the risk of developing lupus by seven-fold, and the risk of developing Sjögren’s syndrome by 16-fold. The C4 alleles that increase the risk for schizophrenia, reduce the risk of developing lupus and Sjögren’s syndrome.
In all three illnesses, the C4 alleles act more strongly in men than in women, providing a possible explanation for the sex differences in the vulnerability of developing the illnesses.
Gene variants determining vulnerability to illness
Banner image credit: Fan Wang Lab
Take a look at our previous top neuroscience stories:
Sign up to receive our latest news
Find out about Scientifica's latest product releases, company news, and developments through a range of news articles, customer interviews and product demonstration videos.

)