
The top neuroscience stories from October 2020
October's best neuroscience stories include the discovery that fear and anxiety share brain circuits, a new approach for analysing the morphology of dendritic spines, and a skin test that could be used to accurately detect Parkinson's disease.
1. What lies between grey and white in the brain
A research team led by the Max Planck Institute for Human Cognitive and Brain Sciences (MPI CBS) has made the superficial white matter, the interface between white and grey matter, visible in the human brain.
Little is known about superficial white matter, due to a lack of methods for studying it in humans, but it is thought to be implicated in conditions such as Alzheimer’s disease and autism.
The new method uses Magnetic Resonance Imaging (MRI) at a very high field strength. The MRI scanner used at the MPI CBS uses a 7 Tesla scanner, compared to typical clinical MRI scanners which work at 1.5 or 3 Tesla. This enables the team to create high resolution maps of the white-grey matter border throughout the entire living human brain.
It is hoped that this new method will provide insights into the organisation of the superficial white matter, for a better understanding of brain development and medical conditions that involve this area of the brain.
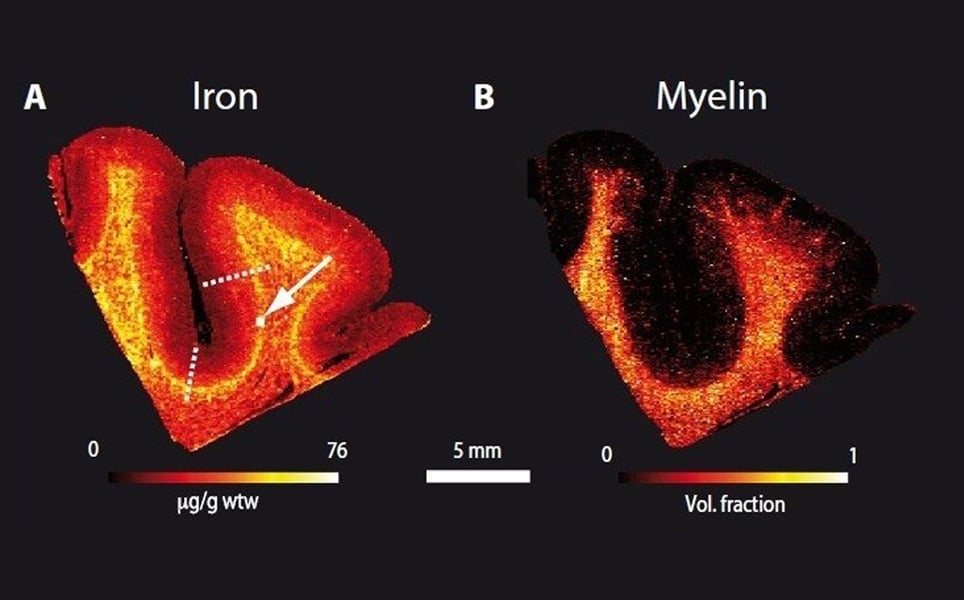
Visualising the superficial white matter
2. Stem cells can help repair spinal cord after injury
Spinal cord injury is often caused by loss of oligodendrocytes, which insulate neurons in myelin sheath, enabling them to effectively transmit signals. By stimulating stem cells in the mouse spinal cord to form large amounts of oligodendrocytes, scientists at the Karolinska Institutet improved nerve function in spinal cord injury.
Stem cells in the adult spinal cord usually become cells that form scar tissue after an injury. However, the researchers found that the cells are not locked into forming scar tissue, and the DNA of the stem cells was receptive to signals that stimulate formation of oligodendrocytes.
It is hoped these findings can one day be applied to humans to stimulate repair following damage to the nervous system.
Spinal cord repair
3. Small brain device proves big game changer for severely paralysed patients
A small brain device, the size of a paperclip, has been successfully implanted in two patients who suffer from severe upper limb paralysis due to motor neuron disease, helping them to text, email and shop online.
The trial, conducted by the University of Melbourne, showed that the device, called Stentrode™ could wirelessly restore the transmission of brain impulses. It was implanted next to the motor cortex via a small keyhole incision in the neck, and through the patients’ blood vessels. Stentrode™ was then used by the patients to control a computer-based operating system, enabling the patients to communicate and control a computer with their minds.
This device restored gave the patients more freedom and independence, by making it possible to control a computer with their minds in their own home.

Restoring paralysed patients' freedom
4. Researchers identify process for regenerating neurons in the eye and brain
Researchers at the University of Notre Dame, Johns Hopkins University, Ohio State University and the University of Florida have identified networks of genes that regulate the process that determines whether neurons will regenerate. This has implications for a range of neurodegenerative disorders which are caused by the death of neurons.
The study has shown that it is possible to regenerate retinal neurons, and the researchers believe that the process for regenerating neurons in the brain will be similar.

Find out more
5. A new approach to analysing the morphology of dendritic spines
Scientists from Peter the Great St. Petersburg Polytechnic University (SPbPU) and UT Southwestern Medical Center have developed a new approach for analysing the shapes of dendritic spines, which have been linked to learning and memory.
These small protrusions from the dendritic membrane of a neuron vary in shape, size and density. When visualising and analysing dendritic spines, scientists usually divide them into three or four subclasses based on their morphology. However, this classification approach doesn’t account for the dynamic nature of the spines, which can change in response to neuronal activity.
The researchers in this study used two-photon, confocal, laser, and super-illumination microscopy to obtain images of spines from cultured neurons, fixed brain slices and intact brain tissue. Through the use of algorithms, they suggest a clusterisation approach to help identify the link between the shape and functions of the dendritic spines, and how this changes during learning and memory and in neurodegenerative disorders.
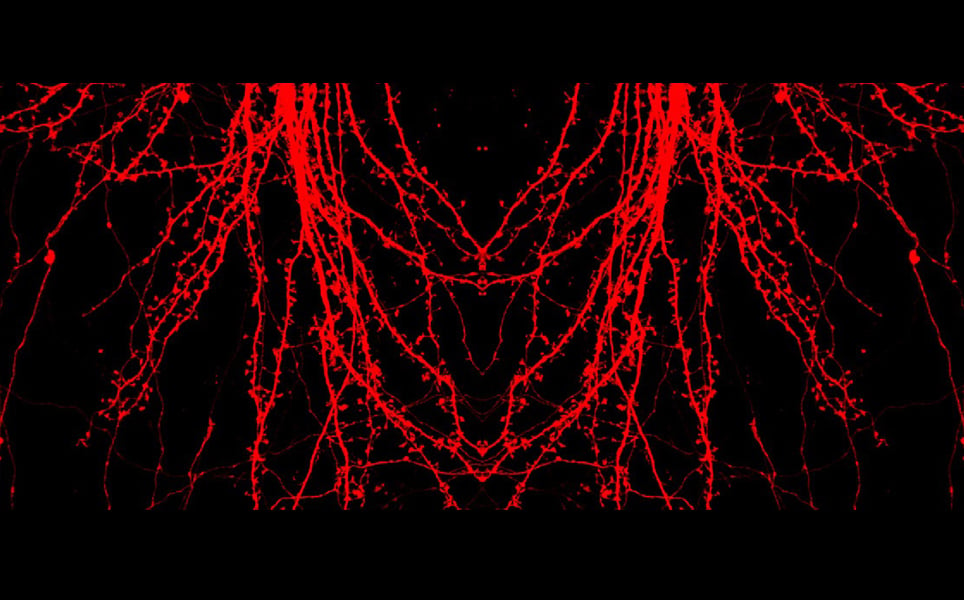
Gaining insight into dendritic spines
6. Fear and anxiety share the same brain circuits
A study led by the University of Maryland and Yonsei University has found evidence that fear and anxiety share brain circuits, contrasting to previous thoughts that fear and anxiety are distinct, with different triggers and brain circuits.
Previously, fear was thought to be controlled by the amygdala, whereas anxiety was thought to be controlled by the bed nucleus of the stria terminalis (BNST). However, using fMRI to examine the neural circuits involved when participants were waiting for certain threats (fear) and uncertain threats (anxiety), the researchers discovered that anticipation of both types of threat activated a common network of core brain regions, including the amygdala and BNST.
These findings could help better understand anxiety and depression, leading to developments of better treatments of these disorders.
Better understanding of fear and anxiety
7. Gut hormone blocks brain cell formation and is linked to Parkinson’s
A structural change to the gut hormone ghrelin has been found by scientists at Swansea University to reduce nerve cell formation and impair memory.
Acyl-ghrelin is known to promote neurogenesis in adult mammals. The change that was investigated by the researchers leads to the formation of two forms of ghrelin – Acyl-ghrelin (AG) and unacylated-ghrelin (UAG). It was discovered that the UAG form of ghrelin reduces nerve cell formation and impairs memory, and that individuals with Parkinson’s disease have a lower blood AG:UAG ratio.
The findings could help develop better treatments for Parkinson’s disease treatments, with UAG being a potential drug target.
Potential Parkinson's target
8. New class of highly effective inhibitors protects against neurodegeneration
Scientists at Heidelberg University have identified that glutamate-activated NMDA receptors can lead to cell death when activated outside of synapses.
When located in synapses, these receptors have roles in learning and memory and neuroprotection. Under normal circumstances, efficient cellular glutamate uptake systems ensure that extra-synaptic NMDA receptors are not activated, therefore nerve cell death is not initiated.
However, in disease states, for example if parts of the brain have reduced oxygen supply following a stroke, glutamate uptake systems are compromised, leading to increased glutamate outside synapses. This increased glutamate activates the extra-synaptic NMDA receptors, causing nerve cell damage and death, leading to reduced brain function.
The researchers identified that extra-synaptic NMDA receptors cause cell death by forming a complex with TRPM4, another ion channel protein. They also developed inhibitors that can disrupt the bond between the proteins, inactivating the ‘death complex’ that they form. These inhibitors appeared to effectively protect nerve cells, eliminating the toxic properties of extra-synaptic NMDA receptors. It is hoped that these inhibitors may offer new treatment options for neurodegenerative diseases that are currently untreatable.
Protecting against neurodegeneration
9. Diagnosing Parkinson’s disease with skin samples could lead to earlier detection
A simple skin test could accurately identify Parkinson’s disease, leading to earlier detection of the disease.
Scientists at Iowa State University found that clumping of the alpha-synuclein protein can be detected in skin samples using a chemical assay - the real-time quaking induced conversion assay. As there is currently no reliable test available, Parkinson’s disease is often misdiagnosed, which has implications for treatments and clinical trials. Earlier and more accurate diagnosis could allow therapies designed to slow or prevent symptom development to be tested, leading to improved treatment options in the future.
Detecting Parkinson's from skin samples
10. Study explains the process that exacerbates MS
Scientists at the Karolinska Institutet have discovered a process that may be responsible for the progressive functional impairment experienced by patients with multiple sclerosis (MS), and also showed how this process can be reversed.
The researchers found that in mice, recovery from MS-like symptoms depends on the ability of microglia to break down damaged cell debris. When researchers removed Atg7, an autophagy gene, the microglia had reduced ability to break down residue created by inflammation. The residue then accumulated over time, which may be a cause for disease progression. Microglia from older mice resembled those from younger mice that lacked Atg7, suggesting this could be why MS progresses with age.
It was also discovered that Trehalose, a sugar derived from plant and funghi., restored the ability of microglia to breakdown myelin residue, preventing disease progression and aiding recovery.
More here
Take a look at our previous top neuroscience stories:
Sign up to receive our latest news
Find out about Scientifica's latest product releases, company news, and developments through a range of news articles, customer interviews and product demonstration videos.

)